Introduction
Epistemological assumptions are defined as the grounds of knowledge that allow one to understand the world and lead to the communication of knowledge to others (Golden & Wendel, 2020). These assumptions involve ideas about the forms of knowledge, how forms of knowledge can be obtained, and what is false or true (Burrell & Morgan, 2006). Epistemological assumptions guide all types of research, either quantitative or qualitative. Positivist epistemological assumptions build quantitative research, while postmodern epistemological assumptions build qualitative research. Positivist epistemological assumptions assume that valid knowledge of the social world is produced by the adherence to scientific methods of natural sciences.
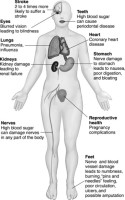
On the other hand, the postmodern epistemological assumption is that knowledge is the product of individual interpretations of the social world (Denzin & Lincoln, 2011). Therefore, epistemology is the nature of knowledge and understanding acquired from different methods of inquiry and investigations. This review will develop epistemological assumptions that will guide qualitative research on the protein-polysaccharides complex to treat diabetes. Diabetes is a physiological condition when the individual's blood glucose level increases (Schwartz et al., 2016; Zhao, Zhang, Pan, Yang, & Jiang, 2021). Diabetes can be categorized into two main types, which are Type-1 diabetes and Type-2 diabetes (Frantz et al., 2018; Pan, Lou, & Wei, 2021). It is seen that the patient who is suffering from Diabetes Mellitus can have vast chances of experiencing immune disorders (Zhou, Chi, Lv, & Wang, 2021). Due to this immune disorder, the whole physiological system cannot respond appropriately (Bossi, Bernardi, Zauli, Secchiero, & Fabris, 2015; Wan et al., 2021). It is worth noting that Diabetes can cause several health issues such as blood flow reduction to the extremities, nerve damage, and the damage exerted in the liver (Figure 1) (Rinaldi et al., 2021; Zilliox, 2021). Many studies postulate that if a diabetic patient can control his or her blood sugar level, that patient can have fewer chances to experience the infectious disorder (Grossmann et al., 2015; Maseko, Staden, & Mhlongo, 2021).
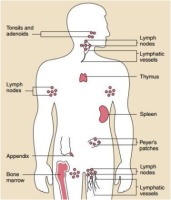
The immune system plays a significant role in the human body, which keeps the body free from any infection (Mannering, So, Elso, & Kay, 2018). The primary function of this system is to protect the body from any foreign substances such as viruses, bacteria, and tumours (Palmer et al., 2015). This system deals with several threats in various ways: engulfing bacteria and killing cysts, parasites, and virus-infected cells (Pan, Lin, Fort, & Patrice, 2021). The main components of the immune system are the thymus, spleen, bone marrow, and lymph nodes (Figure 2) (Pinti et al., 2016).
The thymus is located between the breast bone and the heart. A specific hormone is produced by this organ, which is responsible for the maturation of the immune system's power cells, which are known as lymphocytes (Mahmood, Bari, & Agha, 2016). However, between the diaphragm and the stomach, the spleen is located. The spleen filters the viruses and bacteria out of the lymphocytes and RBC for release as required (Vito et al., 2015). If an infection is contacted with the body, the lymphocytes are released from the spleen to control the disease (Koya et al., 2021). Lymph nodes are seen in various human body parts: groin, armpits, abdomen, neck, chest, and pelvis (Grayson & Kaplan, 2016). The lymph nodes filter the WBC and lymph fluid to attack viruses and bacteria (Cadena et al., 2021; Mahzari, Liu, Arnaout, & Lochnan, 2015).
It has been stated that immune malfunction is occurred due to the disease of Diabetes Mellitus (Zhou et al., 2018). It is seen that high blood glucose unleashes destructive molecules, and for this reason, the natural defences of infection control have interfered with diabetes (Fløyel, Kaur, & Pociot, 2015).
It has been identified that the immune system is altered is innated by the energy imbalance of adipose tissue (Askenasy, 2016; Moreno-Navarrete et al., 2021). The initiating point of this mechanism is white adipose tissue, where the maturing adipocytes and the macrophages are innate as the matured adipocytes, and the macrophages deal with the energy imbalance driven by diet (Hu et al., 2015). The depletion of mature adipocytes is due to the attack of inflammation which is inspired by the macrophage. For this reason, a specific kind of cells is produced which survive the accumulation of lipids per adipocyte in an excessive amount (Palinski & Yamashita, 2015).
Recently, it has been mentioned that a new therapy of utilization regulatory T cells is used in those patients who have Type-1 diabetes for protecting the insulin-producing cells of the pancreas (Goda et al., 2021). The beta-cell autoantigens are glutamic acid decarboxylase, insulin, insulinoma antigen, and tyrosine phosphatase (Maurizi, Guardia, Maurizi, & Poloni, 2018). It is calmed that the autoimmune process of beta-cells, macrophages, beta-cells autoantigens, B lymphocytes, T lymphocytes, and dendritic cells is involved (Martins, 2017). It is essential to determine the factors responsible for causing the immune malfunction in the human body (Alkanani et al., 2015; Torralba-Raga, 2021).
The idea of the necessity of maintaining the blood glucose levels and the immune system so that if any infection is developed in the body of the diabetic patient, then the body can fight against that specific infection. Insulin controls the sugar level in the blood; thus, it is critical to improving the food habits and life cycle. Proper lifestyle can ‘lower the chances of occurrence of diabetes.
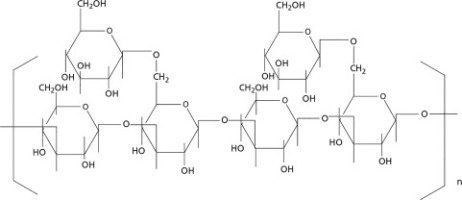
Polysaccharides are identified as valuable compounds in the management of diabetes since they prevent several oxidative stresses and the excess accumulation of reactive oxidants like hydroxyl radical and superoxide that lead to increased lipid peroxidation (Joseph, Panicker, & Janardhanan, 2012; Ojo, Feng, Ojo, & Wang, 2020). Naturally occurring polysaccharides stimulate antioxidant defence in patients by restoring redox balance. Several studies in vivo have proven that polysaccharides protect animals from endogenous antioxidants and reduce the oxidative damage of mitochondrial enzymes and proteins (Joseph et al., 2012). Polysaccharide is the principal active fraction in protein-polysaccharide complexes responsible for anti-diabetic properties (Gao, Kong, Cai, Zhang, & Jia, 2020). Polysaccharides are complex mixtures made up of different molecular weights of monosaccharide constituents (Fig. 3). Polysaccharides in protein-polysaccharide complexes are identified as ideal with anti-diabetic properties since the high and low molecular weight chitosan in the complexes present different or broad-based hypoglycaemic and hypocholesterolaemia effects (Alzahrani, 2017). Further, the different range of molecular weights of polysaccharides presents different therapeutic effects.
Knowledge is created by interpreting previous studies and the creation of questions from sources on the protein-polysaccharides complex. Therefore, adopting postmodern epistemological assumptions that will provide theoretical and empirical knowledge that protein-polysaccharides complex treats diabetes. To achieve this, the research carries out a qualitative investigation of diabetes and the properties of diabetes, treatment requirements, the properties of protein-polysaccharides, and the effects of the protein-polysaccharides complex on the treatment of diabetes an alternative method. Epistemological questions to be answered in this research include diabetes, its conditions, and its symptoms? What drives the need to investigate the treatment of diabetes? What justifies the use of protein-polysaccharides complexes as alternative diabetes therapy treatments? How is the knowledge created in the research justified? In the end, the knowledge created from making connections of the theory will provide understanding on the treatment of diabetes, improving public health in the community.
Epistemological on Diabetes
The widespread changes in dietary habits across the world have led to increased cases of obesity and diabetes. Diabetes is a metabolic disorder characterized by hyperglycaemia leading to the inability of the body to use blood glucose to create energy (Alzahrani, 2017; Association, 2021). There are different types of diabetes, but the most common is Type 1 diabetes and Type 2 diabetes (Association, 2021; Kononenko, Smirnova, Mayorov, & Shestakova, 2020). Type 1 diabetes is an autoimmune condition that causes the body to attack itself, destroying insulin-secreting β-cells (Yadav, Morris, Harding, Ang, & Adams, 2009). Type 1 diabetes occurs suddenly and develops in persons under the age of 30, but Type 2 diabetes, which predominantly occurs in 90-95% of the population with diabetes, starts later in life (Coppieters, Amirian, & Herrath, 2012; Gu et al., 2013; Schmitt, Sanchez, Desobry-Banon, & Hardy, 1998). Type 1 diabetes is mainly managed with insulin since the pancreas cannot produce insulin as the immune system has destroyed the β-cells, and it is common in children since it often starts in childhood (Adams et al., 2011; Yadav et al., 2009). Type 2 diabetes, also referred to as adult-onset diabetes, is characterized by reduced production of insulin quantities by β-cells or the body cells are resistant to insulin (Alexiou & Demopoulos, 2010; Group et al., 2021; Jarald, Joshi, & Jain, 2008). Type 2 diabetes is associated with lifestyle conditions like obese (Teugwa, Boudjeko, Tchinda, Mejiato, & Zofou, 2013). Type 2 diabetes can be managed by exercise, weight loss, and administered oral medication without necessarily using insulin (Adams et al., 2011). The combination of hyperglycaemia and hyperlipidaemia in diabetes causes severe death and morbidity (Dahech et al., 2011). The need to understand hyperglycaemia and hyperlipidaemia in type 2 diabetes or diabetes mellitus is important since the combination of the two conditions in a patient lead to endothelial dysfunction. Endothelial dysfunction is an important hallmark in diabetes mellitus since it signifies the development of cardiovascular disease complications. The prolonged existence of hyperglycaemia, hyperlipidaemia and hyperinsulinemia indicates metabolic markers of complications in diabetes.
Further, hyperlipidaemia and hyperglycaemia are risk factors in the acceleration of diabetes-atherosclerosis (Afshari et al., 2020; Dahech et al., 2011). In an experiment involving non-diabetic and diabetic mice (Dahech et al., 2011), it was observed that glucose promoted protein oxidation and lipid oxidation of Low-Density Lipoproteins (LDL) in vitro. This glucose oxidized LDL led to phosphorylation of extracellular Kinase and Protein Kinase B (Akt) and stimulated macrophages' isolation. The experiment proved that the combination of hyperlipidaemia and hyperglycaemia stimulates macrophage proliferation and causes problems like cardiovascular disease. In addition, the excessive production of reactive oxygen species in diabetic persons leads to oxidative stress, which plays a role in diabetes-associated conditions like fatty liver disease and cardiovascular disease (Dahech et al., 2011). Under these conditions, a high-fat diet complicates the situation from worsening oxidative milieu in cellular functions.
The other problem of treating diabetes with anti-diabetic drugs is that these drugs create adverse effects on other metabolism functions, lead to the supplementation of anti-hyperglycaemia substances that have antioxidant properties, leading to the search for alternative therapies to deal with hyperglycaemia, antiarteriosclerotic, antihypercholesterolemic, antihypertriglyceridemic activities in diabetes (Lee et al., 2010). Diabetes is a risk factor for chronic kidney and atherosclerosis disease (Morton, Liew, Mcdonald, Shaw, & Magliano, 2020). It also causes diabetic renal and cardiovascular complications. This is from the oxidative stress, pathogenic mechanisms, and inflammation stress activities in a diabetic patient (Alzahrani, 2017). This calls for the limitation of oxidative and inflammatory stress in the management of diabetes through the removal of reactive oxygen species. The search for alternative antioxidant therapies is necessary since therapies with vitamin C and E have proven limited in providing benefits in reducing diabetes outcomes in patients (Lee et al., 2010; Mirzavandi, Talenezhad, Razmpoosh, Nadjarzadeh, & Mozaffari-Khosravi, 2020).
For this reason, the antioxidant properties of polysaccharides have been proposed to deal with antiarteriosclerotic, antihypercholesterolemic, antihypertriglyceridemic activities in diabetes. This factor calls for the search for alternative treatment methods for diabetes that reduce the effects of the condition on patients' health. There is a need for glycaemic control in the management of diabetes and the maintenance of good public health. The need for alternative methods arises because popular measures of glycaemic control, including self-monitoring of blood glucose and estimated average glucose (A1c), are not adequate (Albisser, Alejandro, Meneghini, & Ricordi, 2005). This is because the A1c perspective fails to recognize hypoglycaemia in the treatment of diabetes. In addition, self-monitoring of blood glucose (SMBG) lacks the perspective of hypoglycaemia since it simply evaluates the glycaemic status and response of therapy of patients.
Diabetes is a disorder of fat, carbohydrates, and protein metabolism caused by defects in insulin secretion, insulin action or both (Association, 2021; Hu, Li, Zhao, Feng, & Wang, 2010). The disease has high morbidity, mortality, and prevalence rate worldwide, and it has considered incurable but controllable. There are different synthetic drugs and plant remedies used to diminish the consequences of diabetes (Koia & Shepherd, 2020). The role of medicinal plants as sources of hypoglycaemic agents has been studied along with the ethnobotanical and chemical analysis of plants in reducing the effects of diabetes (Alzahrani, 2017). Polysaccharides have been reported to have good hypoglycaemic activity, with many studies finding protein-polysaccharides complexes as ideal hypoglycaemic inducers (Wu et al., 2020).
Epistemological Assumption of Protein-Polysaccharides Complexes
In recent years, many polysaccharides and polysaccharide-protein complexes have been isolated from plants and used as sources of therapeutic ages for conditions like diabetes mellitus (Alzahrani, 2017; Li et al., 2021; Zhao et al., 2021; Zheng et al., 2020). This is because polysaccharides and proteins are the major structural components in food, identified as the leading cause and pathway of diabetes management. Implying the management of food material implies the management of proteins and polysaccharides to manage diabetes (Chen et al., 2020; Schmitt et al., 1998). The interaction between proteins and polysaccharides in complex associative phase separation creates protein-polysaccharide complexes. Protein-polysaccharides complexes form the basis of this research since they have better functional properties than polysaccharides and proteins alone (Alzahrani, 2017; Schmitt et al., 1998). The physical characteristics of the complexes, including structuration or gelation and aggregation, hydration characteristics like viscosity and solubility, and surface properties like emulsifying and foaming, can be used in several areas (Alzahrani, 2017). Among these areas include the microencapsulation, food formulation, synthesis of biomaterials like artificial grafts and edible films, and macromolecular purification required of patients with diabetes.
One of the major plants identified is the mushroom, especially the Agaricus blazei Murrill variety from Brazil. The mushroom variety is selected for it is a basidiomycete brown fungus found in Brazil and Japan, as “Himematsutake” since the mushroom is a source of chemical compounds including polysaccharides, proteins, amino acids, lectins, vitamins, and sterols (Wang, Fu, & Han, 2013). Polysaccharide is identified as an essential chemical compound with immunologic adjuvant characteristics (Han et al., 2021). The compound is vital for it can activate B cells, T cells, NK cells, and other immune cells and promotes the synthesis of IL-1, IL-2, TNF-α, IFN-γ, and NO regulating the creation of antibodies (Wang et al., 2013). The compound is helpful in the body since it complements A. brasiliensis compounds like (Zhang et al., 2021).
Moreover, they act as biological response modifiers (Wang et al., 2013). Fresh mushroom species are identified as the alternative treatment of diabetes since their polysaccharides’ extracts demonstrate antihyperglycemic and antioxidant properties. Polysaccharides are beneficial compounds since they contain bioactivity like antitumor, antiinfection, anticaducity, hypolipidemic, and hypoglycaemia.
Epistemological on Protein-Polysaccharide Complexes Treatment of Diabetes
Fresh mushrooms are recommended as an alternative treatment of diabetes as they have been proven to have antihyperglycemic and antioxidant properties along with polysaccharide extracts (Zahid et al., 2020). Various studies have identified polysaccharides as effective immunity boosters, antioxidants, and antidiabetic (Dahech et al., 2011; Nie et al., 2019). Polysaccharides also are ideal for the treatment of diabetes since they present diverse biological activities and are low cost as therapeutic applications (Alzahrani, 2017; Nie et al., 2019). Protein-polysaccharides complexes from mushrooms possess antihyperglycemic, antilipidemic, and antioxidant properties, making them ideal for the treatment of diabetes (Kaewnarin et al., 2020). Agaricus brasiliensis mushroom variety is rich in protein and polysaccharides, especially the β-glucans variety making it ideal in the treatment of diabetes. Clinical research (Kim, Kim, Choi, & Lee, 2005) proved that β-glucans, polysaccharides, and their enzymatically hydrolysed oligosaccharides from Agaricus brasiliensis create anti-diabetic activities in diabetic rats. The activities include antiarteriosclerotic, antihypercholesterolemic, antihypertriglyceridemic, and antihyperglycemic activities. The clinical trials separated the groups of diabetic rats into four, including the diabetic control group, normal control group, group treated with II (AO), and group treated with I (β-glucans) to identify the different changes to the body from the treatment with Agaricus brasiliensis. The data from this empirical research shows that both β-glucans and AO are highly likely to promote insulin secretion from islets. It also showed that there was high viability and proliferation of islets in normal or diabetic rats. In addition, an empirical study (Oh et al., 2010). Agaricus brasiliensis can treat diabetes since it affects streptozotocin-induced diabetic rats. The research found that the oxidative stress induced by hyperglycaemia leads to the dysfunction of pancreatic β-cells and tissue damage in diabetes mellitus (Oh et al., 2010). The chemical ability of the protein-polysaccharides complexes to deal with hyperglycaemia reduces the dysfunction of pancreatic β-cells and the damage of tissue in patients with diabetes mellitus, thereby making the protein-polysaccharides complex treatment of diabetes. A research carried out (Niwa, Tajiri, & Higashino, 2011) on hypoglycaemia, and antidiabetic efficacy and mechanism of Ipomoea batatas and Agaricus brasiliensis in streptozotocin-induced diabetic rats reveals those hypoglycaemic effects of Ipomoea batatas and Agaricus brasiliensis can suppress the proinflammatory cytokine production and oxidative stress in diabetes and improve pancreatic β-cells mass.
Another source of protein-polysaccharide complexes for the treatment of diabetes includes pumpkins. This complex was identified for its 41.21% polysaccharide component and 10.13% protein component (Li, Zheng, Bukuru, Kimpe, & N, 2004). This combination of protein and polysaccharides is identified as ideal in increasing the levels of serum insulin, the reduction of blood glucose levels, and the improvement of tolerance to glucose in persons with diabetes (Alzahrani, 2017; Fang et al., 2021; Quanhong, Caili, Yukui, Guanghui, & Tongyi, 2005). The consumption of this fruit rich in protein-polysaccharides has been proven to regulate the activity of hypoglycaemia and affect serum insulin levels. The study provided empirical evidence that protein-polysaccharides complex can increase serum insulin levels, reduce blood glucose levels, and improve glucose tolerance (Quanhong et al., 2005). A study found that hypoglycaemic plants like mushrooms and pumpkins are identified as effective and safer treatment modalities for diabetes mellitus, especially in overcoming peripheral insulin resistance (Fang et al., 2021). This is because they have a polysaccharide fraction of G. frondosa (SX fraction) that presented hypoglycaemic action in patients with type 2 diabetes (Konno et al., 2020). Polysaccharides contain Ganoderan A and B, glucans from G. lucidum fruit bodies, β-glucan-protein complex, coriolan and acidic glucuronoxylomannan (Amin & Thakur, 2013; Mootoosamy & Mahomoodally, 2014).
Hence, including mushroom and Cucurbita-derived protein-polysaccharides in the diet may have favourable health effects and reduce the risk of many diseases in the population overall, particularly patients with diabetes which provide understanding on the treatment of diabetes and leads to improve public health in the community.
Conclusion
The epistemological study has led to the identification of knowledge as justified true belief. Evidence and internal inquiry justify the knowledge created or epistemological assumptions or premises leading to logical belief in this research. The knowledge created indicates that premise A (epistemology on diabetes), premise B (epistemology on the protein-polysaccharides complex), premise b acting on premise A leads to the treatment of diabetes in society. The epistemological knowledge is identified as:
1. Diabetes is a single risk condition since the combination of hyperglycaemia and hyperlipidaemia causes severe death and morbidity from conditions like kidney failure and cardiovascular disease.
2. Prolonged hyperglycaemia, hyperlipidaemia, and hyperinsulinemia indicates metabolic problems.
3. Anti-diabetic drugs, on the other hand, create problems in metabolism, supplement hyperglycaemia substances with antioxidant properties causing hyperglycaemia, antiarteriosclerotic, antihypercholesterolemic, antihypertriglyceridemic activities.
4. Protein-polysaccharides complexes are characterized by structuration and aggregation, hydration characteristics including solubility and viscosity, and portray surface properties like foaming properties.
5. Protein-polysaccharides complexes contain polysaccharides that have proven to have hypoglycaemic activity, which minimizes hyperglycaemia leading to an increase in the secretion of insulin and a reduction of blood glucose.
6. Polysaccharides enhance in vitro and in vivo cell-mediated immune response in diabetic patients.
Author contributions
Alzahrani Q and Pinto L - Research concept and design, Alzahrani Q and Pinto L - Collection and/or assembly of data, Alzahrani Q and Pinto L - Data analysis and interpretation, Alzahrani Q and Pinto L - Writing the article, Alzahrani Q and Pinto L - Critical revision of the article, Alzahrani Q and Pinto L - Final approval of the article